If you had not started making shifts toward comprehensive telehealth before the COVID-19 pandemic shutdown, you have to now. Time has run out! Change is hard and dreaded, but it is truly amazing how many new opportunities come with change and how much we grow. The American Medical Association estimates that 75% of physician, urgent care, and emergency room visits can be handled safely and effectively with a telehealth visit. During the COVID-19 pandemic shutdown, we have seen even more services and specialties opt to start offering telehealth visits. I have had nutrition counseling, physical therapy, and primary care services all virtually, and I am sure others have had even more.
Many are delaying shifting facilities to accommodate telehealth because they are overwhelmed by creating the perfect environment for providers and patients. In the end, waiting to execute a telehealth facilities plan until it is absolutely perfect will just hinder the transition. Some basic concepts can be implemented, tested, and improved upon continuously until your organization finds what works best for you in your current facilities and can inform new facilities being planned.
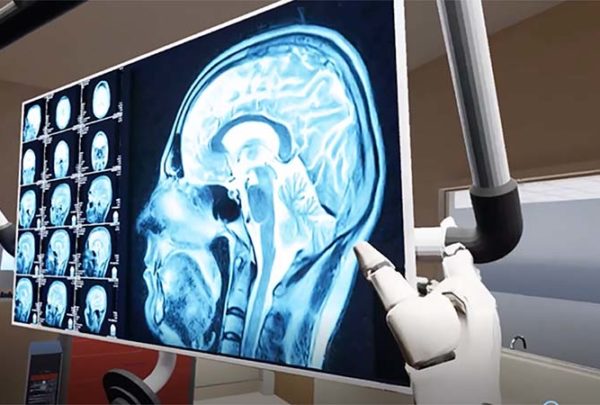
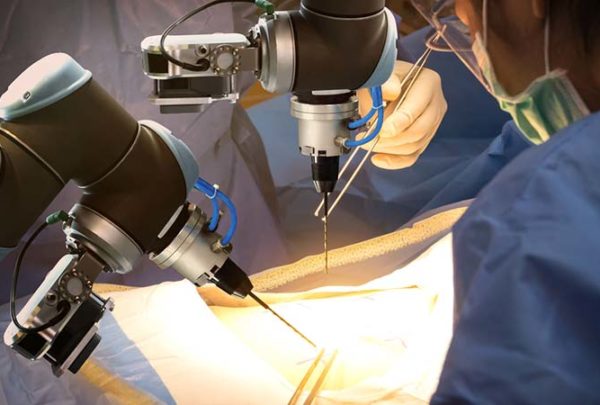
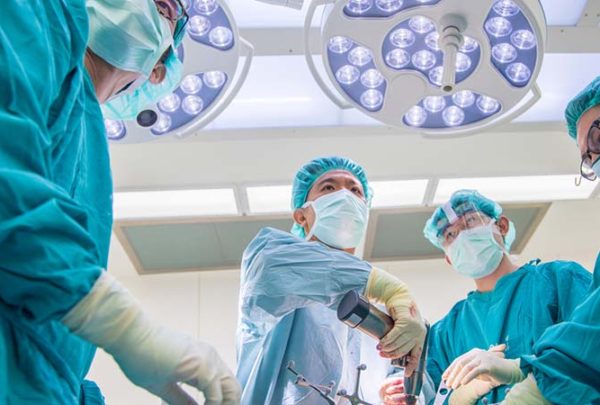
There are two general types of telehealth visits. The first is what we were thrown into during this pandemic, where patients stay home and connect to their provider via a computer or handheld device while the provider is in the office or even their home. The second is where the patient is in the exam room with a nurse or a provider and they connect with a specialty provider virtually. Which is appropriate depends on the health concern at hand.
Considerations for Provider Telehealth Spaces
- Use offices or micro-offices with video and workstations. While physician offices are acceptable, shared provider workrooms are increasing in lieu of offices. In this case, micro-offices with sliding doors and an area about 60 NSF work great. Micro-offices can also be a branding opportunity for organizations.
- Use a clean backdrop with a branding image. Light blue works well as a background color, but keep the rest of the walls light in color.
- Avoid top-down lighting and backlighting. Use lighting in front of the provider near the ceiling to avoid shadows.
- Ensure adequate STC ratings of walls to minimize noise interference
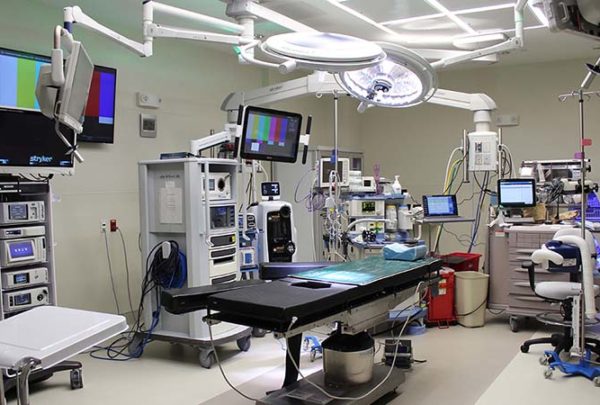
Considerations for Telehealth Exam Rooms
- Exam chairs in lieu of exam tables
- Virtual connections
- Wall-mounted workstations in exam rooms, especially if swing arms are installed
- Mobile carts that can travel to any room if the connections are installed in the rooms and allow for dynamic exams
- iPad or other handheld device
- Diffuse lighting in front of patient (avoid top-down lighting), but the in-room nurse or provide may need to use a movable exam light or headlamp to visualize specific issues
- Light and bright walls that do not create color rendition on skin or clothing. It’s best if the paint has a matte finish (no gloss) to reduce glare.
- Minimize windows or utilize black-out shades to minimize the “identify protection program appearance”
- Adequate STC ratings for doors and walls to minimize noise interference and for HIPAA compliance
- Sinks still need to be located in rooms.
So what does a significant shift mean for ambulatory facilities in the future? Some studies say there could be a 25-30% reduction in required exam and support spaces. In reality, this all depends on the population, specialties, and acuity of patients being served. If anything, it stresses the need for:
- Flexible spaces that can accommodate walk-in appointments and virtual appointments
- Improved infrastructure to handle increased electrical loads, redundant backup power, and automatic transfer switching for smooth uninterrupted service
- Improved IT and cybersecurity
- Right-sized rural facilities that can financially benefit organizations with pressured reimbursements
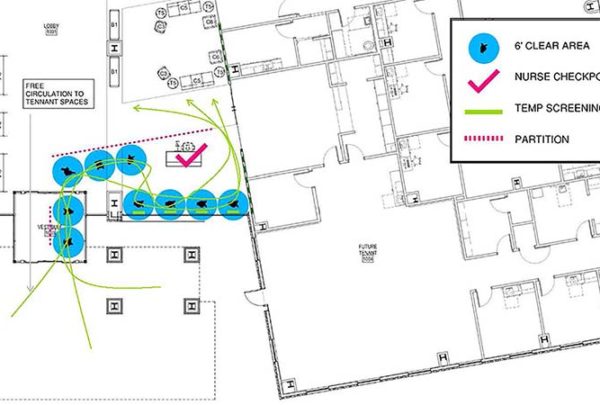
- Shift in “check-in” process where the scheduler calls before a visit to review basic patient information, reason for visit, and insurance. This is likely followed by a nurse-provider consult to communicate patient information. Getting and communicating vitals is a challenge since patients might not have access to scales, thermometers, etc.
- Increased productivity of providers since telehealth visits take less physician time
- Fewer visits to clinics from patients located in long-term acute care hospitals, nursing homes, rehab facilities, detention centers, etc.
- Increased use of collaborative spaces, huddle rooms, and staff consult rooms
Aside from the physical implications of moving to telemedicine, a host of other operational and strategic challenges need to be addressed, such as staffing, reimbursements, payments, protocols, telehealth-appropriate patients and visits, and schedules. If there is any advice or encouragement it’s this: Change is good, and it’s going to be constant, fast, and exciting. Embrace it to succeed.